Concise Communication
Impact of antimicrobial use in dogs on antimicrobial resistance and shared flora with human owners
- Kirthana Beaulac, Claire L. Fellman, Annie S. Wayne, Laura A. McDermott, David R. Snydman, Shira Doron
-
- Published online by Cambridge University Press:
- 09 January 2023, e1
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Transmission of bacteria between animals and humans in domestic households is increasingly recognized. We evaluated the presence of antimicrobial-resistant fecal bacteria in 8 dog-owner–dog pairs before and after the dog received amoxicillin-clavulanate. The study identified shared flora in the humans and dogs that were affected by antimicrobial administration.
Antibiotic Stewardship
SG-APSIC1059: Impact of a single intervention as part of a antimicrobial stewardship in a surgical unit of a tertiary-care referral center for neurosurgery
- Kavita Raja, Dinoop Korol Ponnambath, Shiny Biju, Jyothi Embekkat Kaviyil
-
- Published online by Cambridge University Press:
- 16 March 2023, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobial resistance is a worldwide problem leading to increasing deaths due to intractable infections, especially in postoperative patients who have extended stays in ICUs due to other surgical complications. Carbapenem and colistin resistance has been increasing here; hence, it was decided to monitor and control antibiotic use. In the neurosurgery unit of a quaternary-care hospital in South India, surgical prophylaxis was chosen as less problematic area in which to implement antibiotic stewardship. Objective: To study the difference in the antibiogram pattern of isolates from neurosurgery postoperative patients, before and after the introduction of a surgical antimicrobial prophylaxis policy from the UK National Health Service (NHS). Methods: After the implementation of a new surgical prophylaxis protocol taken from the UK NHS guidelines, we studied its impact by analyzing the antibiogram before implementation (period 1 from January 1, 2020, to December 31, 2020) and after implementation (period 2 from April 1, 2021, to September 30, 2021). This period corresponded to the same number of isolates as the earlier period. Antibiogram criteria: All clinically relevant infections due to the ESKAPE pathogens were included in the antibiogram. The antibiotics analyzed included β-lactams, cephalosporins, β-lactam- lactamase combinations, carbapenems, aminoglycosides, colistin and tigecycline for gram-negative bacilli and penicillin, oxacillin, aminoglycosides, vancomycin, and linezolid for gram-positive cocci. For analysis, the difference was deemed significant according to the criteria stated in CLSI document M39-A4 (4th edition, January 2014). Results: In period 1, 170 isolates were tested, and in period 2, 162 isolates were tested. Among the isolates, Enterococcus spp and Enterobacter spp were too few in number for a comparison. For the gram-negative bacilli, E. coli, Klebsiella pneumoniae, and Acinetobacter baumannii, the differences were significant for the β-lactam–lactamase combinations, carbapenems, and amikacin, with higher susceptibility in period 2. For Staphylococcus aureus, oxacillin, erythromycin, and clindamycin showed a significant increase in susceptibility in period 2. Relevant tables and a graph will be included in the presentation with detailed discussion. Conclusions: Controlled surgical prophylaxis strictly implemented can lead to a significant change in the antibiotic susceptibility pattern among isolates causing healthcare-associated infections among postoperative patients in intensive care units.
Poster Presentation - Top Poster Award
Antibiotic Stewardship
Clinical factors and diagnoses associated with inappropriate urine-culture ordering in primary care
- Marissa Valentine-King, Barbara Trautner, Roger Zoorob, Michael Hansen, Jennifer Matas, Robert Atmar, Larissa Grigoryan
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Inappropriate urine-culture ordering is associated with increased antibiotic prescribing in myriad care environments, including acute and long-term care. In primary care, where urinary tract infections (UTIs) are commonly encountered, the appropriateness of urine-culture ordering has not been well described. We examined the appropriateness of urine-culture ordering and factors associated with inappropriate urine-culture ordering in primary care. Methods: We conducted a secondary analysis of data from a previous prospective study that included patients aged ≥18 years presenting with provider-suspected UTI with an accompanying urine culture at 2 safety-net, primary-care clinics in Houston, Texas, between November 2018 and March 2020. Patients with complicated or uncomplicated UTI were included, but those with a urinary catheter and pregnant females were excluded. Urine cultures were considered appropriate if the patient had an evidence-based symptom of UTI (ie, dysuria, frequency, urgency, hematuria, fever, chills, costovertebral angle tenderness, suprapubic, pelvic, or flank pain, or nephrolithiasis) as a diagnostic code or listed in providers’ free-text documentation. Diagnostic codes for symptoms that were not evidence based were grouped into categories based on body system, visit type (eg, routine visit), or sign or symptom clusters. We evaluated the relationships among demographic and clinical factors, the clinic visited, and non–evidence-based diagnostic codes with inappropriately ordered cultures. Results: We examined 870 cultures from 807 patients. Overall, 61.5% of patients were Hispanic (61.5%) and 23% were African American or Black. Also, 70.6% were women; the mean age was 49.2 years (SD, 14.6); and the mean Elixhauser score was 1.9 (SD, 5.4). Among the 870 cultures, 210 (24%) were ordered inappropriately. Dysuria (n = 289), frequency (n = 129), and UTI or cystitis (n = 117) were the most common, evidence-based codes among appropriate cultures. In the adjusted model, the nonteaching clinic (aOR, 6.33) and diagnostic codes comprising the following categories were associated with inappropriate culturing: acute lower back pain (aOR, 5.42), cardiac-related visits (aOR, 2.41), urinary incontinence (aOR, 4.46), routine health visits (aOR, 3.66), urine characteristics (aOR, 14.32), voiding difficulties (aOR, 3.88), and well-woman visits with a gynecological exam or family planning aspect (aOR, 12.27) (all P < .05). Conclusions: This research highlights potential gaps or miscues in provider behavior related to urine culture ordering, and unveiled problematic culturing related to urine characteristics and to routine visits, especially of a gynecological nature. This information can be incorporated into diagnostic stewardship interventions to address misconceptions, and to further explore the reasoning or processes wherein urine cultures are ordered for routine visits.
Financial support: NIAID UM1AI104681
Disclosure: None
Letter to the Editor
Increase in the incidence of Candida parapsilosis and Candida tropicalis bloodstream infections during the coronavirus disease 2019 (COVID-19) pandemic
- Thanus Pienthong, Suttichai Visuttichaikit, Piyaporn Apisarnthanarak, Kittiya Jantarathaneewat, David J. Weber, Anucha Apisarnthanarak
-
- Published online by Cambridge University Press:
- 10 January 2023, e2
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Poster Presentation - Top Poster Award
Antibiotic Stewardship
Impact of the COVID-19 pandemic on inpatient antibiotic use in Indonesia and the Philippines
- Amara Fazal, Olivia McGovern, Garrett Mahon, Fernanda Lessa, Ma Tarcela Gler, Jemelyn Garcia, Mark Festin, Kuntaman Kuntaman, Ida Parwati, Cherry Siregar, Jay Christian, Gina de Guzman Betito, Maya Montemayor, Arleen De Leon, Emmeline Borillo, Mark Llanes, Regina Berba, Musofa Rusli, Farizal Rizky, Mariyatul Qibtiyah, Bambang Semedi, Rosantia Sarassari, Leonardus Widyatmoko, Basti Andriyoko, Adhi Sugianli, Dewi Turbawaty, Ivo Ranita, Franciscus Ginting, Made Krisna, Rahmadania Marita Joesoef, Twisha Patel
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s1-s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
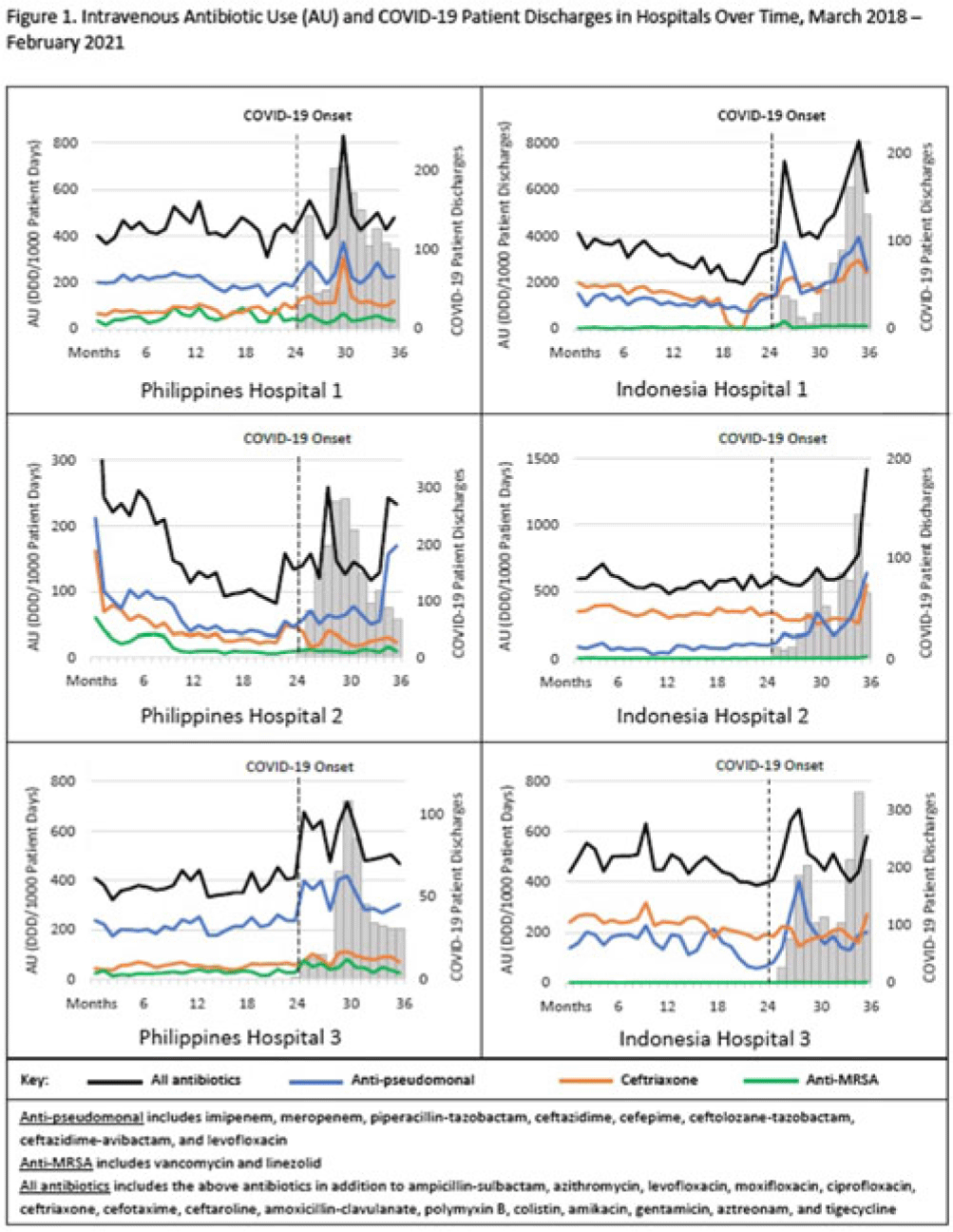
Background: The coronavirus disease 2019 (COVID-19) pandemic severely affected Southeast Asia, with >35 million cases and ~360,000 deaths. Despite relatively low rates of secondary bacterial infection among inpatients with COVID-19, several countries reported increased antibiotic use; raising concerns for worsening antimicrobial resistance. We assessed the impact of the COVID-19 pandemic on the use of antibiotics commonly used to treat respiratory infections in Southeast Asia. Methods: We evaluated intravenous antibiotic use among hospitalized adults in acute-care wards in 6 hospitals; 3 in Indonesia and 3 in the Philippines. We abstracted data on antibiotics that are commonly used to treat respiratory infections in these hospitals. We calculated antibiotic use rates for the 25 included antibiotics as monthly defined daily dose per 1,000 patient days (or patient discharges where patient days was unavailable) using data from pharmacy dispensing records and administrative records. Median antibiotic use rates for the prepandemic period (March 2018–February 2020) and the pandemic period (March 2020–February 2021) were compared, and percentage changes were calculated for (1) all 25 antibiotics combined; (2) ceftriaxone; (3) vancomycin and linezolid combined (anti-MRSA); and (4) broad-spectrum antibiotics with activity against Pseudomonas aeruginosa (anti-PSA). Monthly antibiotic use and COVID-19 patient discharges were graphed over the 36-month study period (March 2018–February 2021) to visualize trends (Fig. 1). The Wilcoxon rank-sum test was used to determine whether differences in median antibiotic use rates were statistically significant (2-tailed P < .05). Results: Overall, trends in antibiotic use were higher during months with increased COVID-19 patient discharges (Fig. 1). Use of all 25 antibiotics combined significantly increased in 4 of 6 hospitals (6.9%–63.6%) during the pandemic period compared to the prepandemic period. Ceftriaxone use significantly increased in 3 of 6 hospitals (37.1%–55.4%) and decreased in 3 of 6 hospitals (15.9%–31.9%). Anti-PSA antibiotic use significantly increased in 4 of 6 hospitals (16.1%–161.5%). Although anti-MRSA antibiotic use was low (comprising <2% of the overall included antibiotic use in Indonesia and <11% in the Philippines), use during the pandemic increased in 3 of 6 hospitals (59.8%–212.6%). Conclusions: We observed substantial increases in antibiotic use among hospitalized adults in Indonesia and the Philippines during the COVID-19 pandemic. The increased use of broad-spectrum antibiotics is concerning given the potential consequence of worsening antimicrobial resistance. Understanding how increases in antibiotic use compares to rates of bacterial infection, antimicrobial resistance, and antibiotic availability and accessibility during this time is important to contextualize results. These findings reinforce the importance of antibiotic stewardship practices to optimize antibiotic use, especially during pandemics.
Disclosure: None
Antibiotic Stewardship
SG-APSIC1093: Engaging inpatients in antibiotic stewardship efforts: The need to enhance knowledge and increase involvement in their antibiotic therapy
- Evonne Tay, Angela Chow
-
- Published online by Cambridge University Press:
- 16 March 2023, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objectives: In tertiary-care settings, up to 50% of patients are prescribed at least 1 antibiotic. However, patients are often not proactively provided with information nor involved in shared decisions regarding their antibiotic therapies. Understanding inpatients’ knowledge and the extent of their involvement in antibiotic therapy help reduce inappropriate or unnecessary antibiotic use. Methods: A cross-sectional survey was conducted from March to December 2021 in a 1,600-bed, adult, acute-care, tertiary-care hospital. Patients prescribed antibiotics for the past 1 week during their hospital stay were surveyed. Ten questions assessing patients’ knowledge of their antibiotic therapy and 3 questions adapted from the NHS Care Quality Commission Inpatient survey (2013) were included in the survey questionnaire. Results: Among the 323 patients surveyed, 88% knew that they had been given antibiotics, and 80% felt that it was important to be informed of the reason, 76% felt that it was important to be informed of side effects, 74% felt that it was important to be informed of duration, and 72% felt that it was important to be informed of dosing frequency. However, only 71% knew the dosing frequency, 54% knew the side effects, 37% knew the duration, and 13% knew the name of the antibiotic agent administered. Of those unaware of the antibiotic name, 59% had indicated their desire to know. Among those aware of their antibiotic therapy, 85% had trust in their doctors but only 42% felt that they always received answers to their questions on antibiotics in an understandable manner from their doctors. Furthermore, 41% felt that they were often or always not given enough time to question their doctors. To raise their awareness on antibiotic use, 73% of respondents felt that having protected time with the doctors to understand more about their antibiotic therapy would be effective. Conclusions: Most inpatients lacked knowledge of details of their antibiotic therapy, and fewer than half were involved in it. Allocation of protected time with doctors to understand their antibiotic therapy can be a potentially effective strategy to increase patient engagement to enhance hospital antibiotic stewardship efforts.
Original Article
Going local: Evaluating guideline adherence and appropriateness of antibiotic prescribing in patients with febrile neutropenia at an academic teaching hospital
- Rachel Liu, Melissa R. Gitman, Andrew M. Morris, Miranda So
-
- Published online by Cambridge University Press:
- 09 January 2023, e3
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Febrile neutropenia (FN) is a medical emergency with significant morbidity and mortality for oncology patients, requiring comprehensive workup and timely antibiotic administration. We evaluated concordance with locally developed FN guidelines and outcomes of cancer patients admitted to general internal medicine at an academic teaching hospital.
Methods:We conducted a retrospective observational cohort study of patients admitted between July 1, 2016, and June 30, 2017, for FN. Patients were classified as having low-risk or high-risk FN according to their malignancy and chemotherapy. Primary outcome was the proportion of patients receiving guideline-concordant antibiotics within 48 hours of admission to general internal medicine. Secondary outcomes were the proportion of patients in whom empirical antibiotics were active against pathogens isolated, rate of antibiotic-associated adverse events, and in-hospital mortality. We used logistic regression to model relationship between FN risk and guideline-concordant antibiotics.
Results:Among 100 patients included, 34 (34%) were low-risk FN and 66 (66%) were high-risk. Proportion of guideline-concordant empirical antibiotics was significantly lower among low-risk FN patients than high-risk patients: 12 (35%) of 34 versus 47 (71%) of 66 (P = .001). Empirical antibiotics were active against 17 (94%) of 18 isolated pathogens. The mortality rate was 3%, and 16% of patients experienced antibiotic-associated adverse events. Hematological malignancy and infectious diseases–trained physician involvement were associated with guideline-concordant prescribing, with adjusted odds ratios of 3.76 (95% CI, 1.46–9.70; P = .006) and 3.71 (95% CI, 1.49–9.23; P = .005), respectively.
Conclusions:Guideline concordance was low compared to published reports. Factors influencing appropriate antimicrobial prescribing in patients with FN warrant further exploration.
Antibiotic Stewardship
SG-APSIC1101: Virulence factors and antimicrobial resistance in coagulase-negative staphylococci isolated from blood of neonates
- Svetlana Kolesnichenko, Irina Kadyrova, Alyona Lavrinenko, Lyudmila Akhmaltdinova, Lyudmila Panibratec
-
- Published online by Cambridge University Press:
- 16 March 2023, pp. s1-s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objectives: To determine virulence genes and sensitivity to antibacterial drugs of Staphylococcus epidermidis isolated from blood cultures of newborns. Methods: A study of сoagulase-negative Staphylococcus (CoNS) from newborns with sepsis was conducted in the regional perinatal center in Karaganda, Kazakhstan. Blood-culture identification was performed using MALDI-TOF MS. Virulence factors were determined on primers (sdrG, sdrG, atl, lip, nuc, ebh, hlb, sspA, sspB, and gehD) with PCR (Bio-Rad CFX 96). Susceptibility to antibiotics determination was carried out using the disc-diffusion method. Testing with cefoxitin was used to detect methicillin resistance in staphylococci. Results: Overall, 18 Staphylococcus epidermidis isolates from blood cultures of newborns with sepsis were investigated from January to December 2021. The frequency of detection of virulence genes was distributed as follows: atl (94.5%), sspB (94.5%), sspA (89%), gehD (89%), ebh (89%), hlb (72%), sdrG (39%), sdrF (28%), nuc (28%), and lip (13%). Also, 10 isolates (55%) were resistant to cefoxitin (MRSE). Furthermore, 72% of S. epidermidis isolates showed resistance to azithromycin and 33% were resistant to clindamycin and gentamicin. Also, 39% of strains were resistant to fluorchinolones. All isolates were susceptible to vancomycin, linezolid, and fusidic acid. Conclusions: S. epidermidis strains isolated from blood cultures had high rates of exoenzymes sspB, sspA, gehD, autolysin (atl), β-hemolysin (hlb), and cell-wall–associated fibronectin-binding protein (ebh). Among 18 neonatal sepsis pathogens, 10 (55%) were MRSE, so it is necessary to pay attention to antibiotic therapy adjustment.
Poster Presentation - Top Poster Award
Antibiotic Stewardship
Multi-faceted approach to decreasing inappropriate antibiotic prescribing for viral upper respiratory tract infections
- Jamilah Shubeilat, Dan Ilges, Angie Ton, Angela Huang, M. Teresa Seville
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
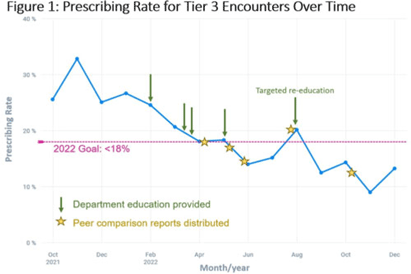
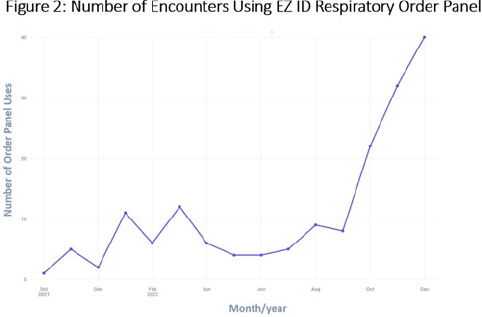
Background: Prescribing of antibiotics for viral upper respiratory infection (URI) remains a pressing public health problem. We sought to reduce inappropriate prescribing of antibiotics for viral URIs at primary-care practices at Mayo Clinic Arizona (MCA). Methods: Diagnostic codes for URIs commonly caused by viruses were categorized as tier 3 (ie, never prescribe). The inappropriate prescribing rate was defined as the number of tier 3 encounters resulting in a prescription for a URI antibiotic divided by the total number of tier 3 encounters. MCA primary-care departments, including family medicine, community internal medicine, emergency medicine, and women’s health internal medicine, were included in the intervention. Each department was briefed on the project, including baseline department prescribing data, and was provided education. Education topics included appropriate indications for antibiotics, patient-centered strategies for reducing antibiotic use, and a review of electronic resources developed specifically for the project. Resources included a syndromic ambulatory order panel (EZ ID Respiratory Order Panel) and a viral prescription pad, which contains simplified over-the-counter recommendations for symptomatic management of viral URIs and patient education. Quarterly peer comparison reports were provided to the department chairs and/or site leads. Our goal was to reduce inappropriate prescribing by 22% in 2022. An Epic dashboard (SlicerDicer model) was developed to track data on an ongoing basis. We used χ2 tests to compare categorical variables. Results: Department education was completed by June 2022 (Fig. 1). The annual antibiotic prescribing rate for tier 3 encounters decreased by 29% from a baseline rate 23.6% in 2021 to 16.4% in 2022 (P < .001). The posteducation prescribing rate (June 2022–December 2022) was 13.1%. Utilization of the EZ ID ambulatory order panel increased from an average of 1.5 uses per month in 2021 to 13.3 uses per month in 2022 (Fig. 2). Repeated healthcare contact for URIs within 14 days of tier 3 encounters did not differ among patients prescribed and not prescribed an antibiotic in all of 2022 (3.8% vs 3.9%; P = .91) or during the posteducation period (1.8% vs 4.2%; P = .14). There was no appreciable diagnostic shift over the course of 2022 (Fig. 3). Conclusions: A multifaceted intervention, which included baseline education, promotion of syndrome-specific order panels, dissemination of resources for symptomatic management, and distribution of peer comparison reports, resulted in significant reduction of inappropriate antibiotic prescribing for URIs.
Disclosure: None
Antibiotic Stewardship
SG-APSIC1074: Trend of ‘ESKAPE’ and their susceptibility changes for meropenem and levofloxacin during the pandemic at Sardjito Hospital Yogyakarta Indonesia
- Andaru Dahesihdew, Yunan Nadhif Fanani
-
- Published online by Cambridge University Press:
- 16 March 2023, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objectives: The bacteria in the ‘ESKAPE’ group are monitored due to their ability to resist antibiotic action. During the COVID-19 pandemic at our hospital, the usage of meropenem and levofloxacin as the empirical treatment for bacterial pneumonia increased and might have contributed to the antimicrobial resistance problem. In this study, we evaluated the ESKAPE group infection rates and their susceptibility to antibiotics in Dr. Sardjito Hospital, a referral and academic hospital in Yogyakarta, Indonesia. Methods: Data for ESKAPE pathogens in 2019–2021 were taken from the microbiology laboratory of Dr. Sardjito Hospital and were evaluated. Results: The proportion of ESKAPE isolates among positive cultures during 2019–2021 slightly increased from 49.4% to 48.4% to 50.7% each year (P > .05). The dominant ESKAPE infections were pneumonia, bloodstream infection, and urinary tract infection by K. pneumoniae, and wound infection by P. aeruginosa. The susceptibility pattern of ESKAPE to meropenem decreased from 72% in 2019 to 68% in 2020 but increased to 84% in 2021. To levofloxacin, the susceptibility pattern was decreased in a fluctuating trend from 68% in 2019 to 33% in 2020 and to 39% in 2021. During the COVID-19 pandemic (2020–2021), the pattern of ESKAPE infections was similar to that of 2019. In descending order, the frequency rank was K. pneumoniae, P. aeruginosa, A. baumannii, Enterobacter spp, and S. aureus. The proportions of MDR isolates increased from the prepandemic period to the COVID-19 pandemic era for E. faecium (from 5% to 24.4%), for A. baumannii (from 9.6% to 38.5%), and for P. aeruginosa (from 7.4% to 13.5%) (P < .05). These patterns did not differ between non–COVID-19 patients and COVID-19 patients. These results highlight the general impact of overused antibiotics beyond COVID-19 patients. Usage of watched and restricted antibiotics must be more controlled because bacterial coinfection and superinfection in COVID-19 patients was relatively low. Conclusions: During the COVID-19 pandemic, ESKAPE infections increased and their susceptibility to meropenem and levofloxacin decreased. Tight control of antibiotic usage is needed.
Commentary
Bacteriuria in older adults triggers confusion in healthcare providers: A mindful pause to treat the worry
- Eva M. Amenta, Robin L.P. Jump, Barbara W. Trautner
-
- Published online by Cambridge University Press:
- 09 January 2023, e4
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The evidence base for refraining from screening for or treating asymptomatic bacteriuria (ASB) in older adults is strong, but both practices remain prevalent. Clinical confusion over how to respond to a change from baseline, when to order a urinalysis and urine culture, and what to do with a positive urine culture fuels unnecessary antibiotic use for ASB. If the provider can take a mindful pause to apply evidenced-based assessment tools, the resulting increased clarity in how to manage the situation can reduce overtreatment of ASB.
Poster Presentation - Top Poster Award
Antibiotic Stewardship
Description of antibiotic stewardship expertise and activities among US public health departments, 2022
- Destani Bizune, Angelina Luciano, Melinda Neuhauser, Lauri Hicks, Sarah Kabbani
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s3
-
- Article
-
- You have access Access
- Open access
- Export citation
-
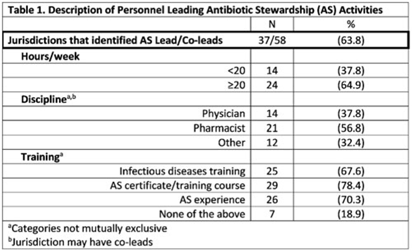
Background: In 2021, the CDC awarded >$100 million to 62 state, local, and territorial health departments (SLTHDs) to expand antibiotic stewardship expertise and implement antibiotic stewardship activities in different healthcare settings. Our objective was to describe SLTHD antibiotic stewardship personnel and activities to characterize the impact of the funding. Methods: SLTHDs submitted performance measures, including quantitative and qualitative responses, describing personnel supporting antibiotic stewardship activities, types of activities, and healthcare facilities and professionals engaged from January through June 2022. A quantitative analysis of performance measures and qualitative thematic analysis of select narrative responses are reported. Results: Most SLTHDs (58 of 62, 94%) submitted performance measures. Among them, 37 (64%) reported identifying an antibiotic stewardship leader or coleader; most were pharmacists (57%) or physicians (38%) with infectious diseases training (68%) (Table 1). Of the remaining STLHDs, 20 reported barriers to identifying a leader or coleader, including hiring process delays and programmatic barriers (Table 2). SLTHDs reported 254 antibiotic stewardship activities; most reported activities involving multiple activity types (44%). Education and communication (eg, providing stewardship expertise) was the most common single activity (30%), followed by antibiotic use tracking and reporting (13%), assessment of antibiotic stewardship implementation (8%), and action and implementation (eg, audit and feedback letters) (4%). The highest number of activities were implemented in multiple healthcare settings (35%), followed by acute care (21%), outpatient (18%), long-term care (17%), and other (9%) (Fig. 1). SLTHDs reported engaging 4,970 healthcare facilities and 15,194 healthcare professionals in antibiotic stewardship activities across healthcare settings, to date, as part of this funding opportunity (Fig. 2). Conclusions: Antibiotic stewardship funding to SLTHDs allowed for increases in capacity and expanded outreach to implement a variety of antibiotic stewardship activities across multiple healthcare settings. Sustaining STLHD antibiotic stewardship activities can help increase engagement and coordination with healthcare facilities, healthcare professionals, and other partners to optimize antibiotic prescribing and patient safety.
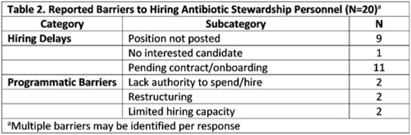

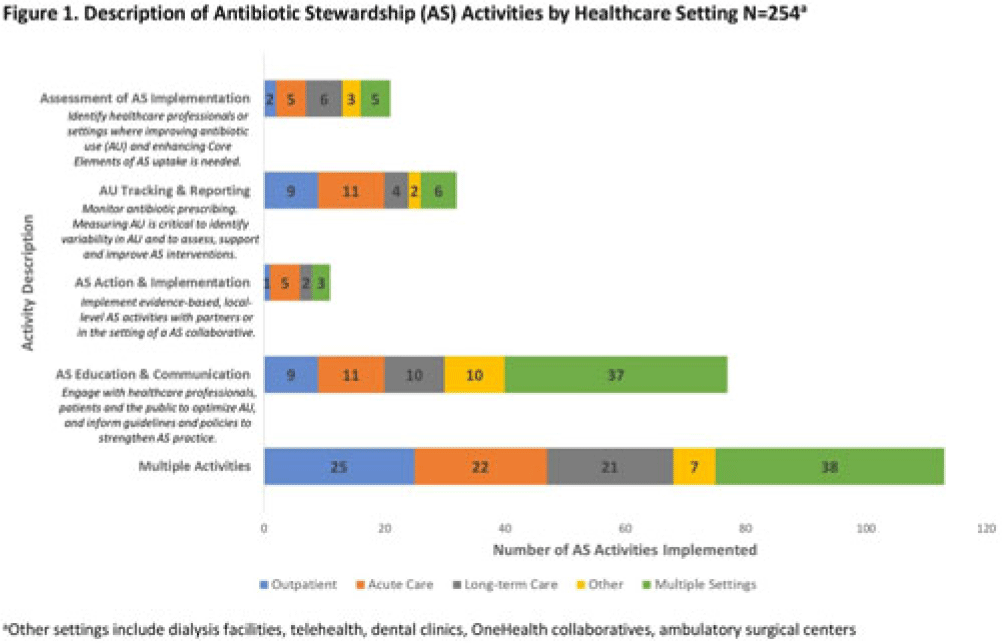
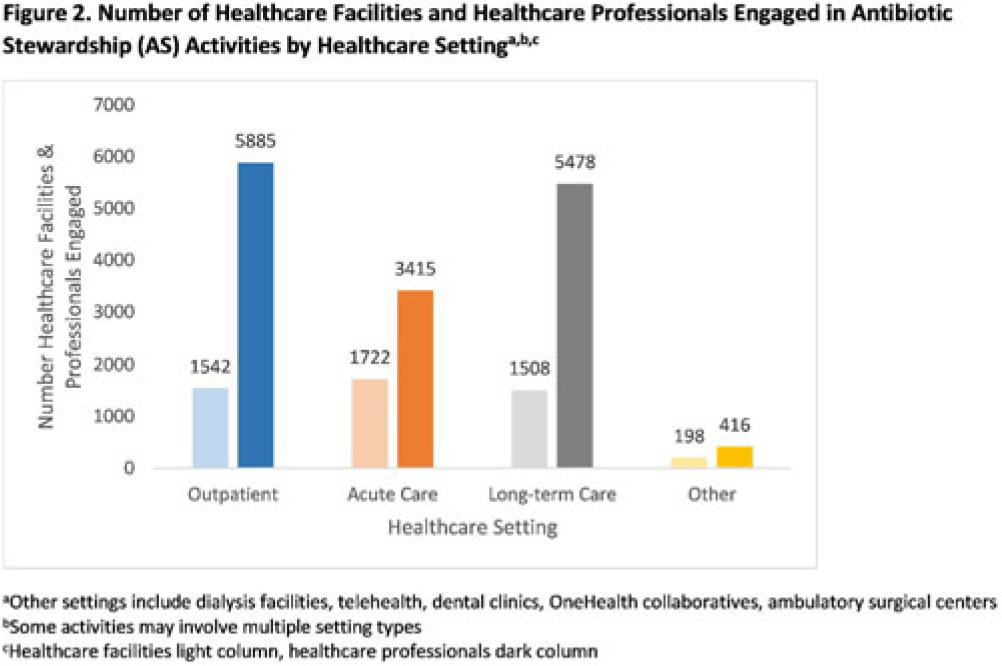
Disclosure: None
Fear of missing organisms (FOMO): Diabetic foot and osteomyelitis management opportunities
- Morgan Morelli, Andrea Son, Yanis Bitar, Michelle Hecker
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s3-s4
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospitalizations for diabetic foot infections and lower-extremity osteomyelitis are common. Use of empiric antibiotic therapy for methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa is also common. Guidelines recommend antibiotic therapy based on severity of illness, risk factors for MRSA and P. aeruginosa, and local prevalence. We evaluated the concordance between empiric antibiotic therapy and both culture results and definitive antibiotic therapy with a focus on MRSA and P. aeruginosa. We also evaluated how well MRSA and pseudomonal risk factors were predictive of culture results with these organisms. Methods: We conducted a cohort study of all patients admitted to our hospital system in 2021 with a diagnosis of a diabetic foot infection or lower-extremity osteomyelitis. Patients were included if they had an International Classification of Disease, Tenth Revision (ICD-10) diagnosis code of M86, E10.621, E11.621, or E08.621. Patients were excluded if antibiotics were for another indication or if they were aged <18 years. In patients with multiple hospitalizations only the first hospitalization was included. Empiric antibiotic therapy included antibiotics started by the admitting team. Definitive antibiotic therapy included the final antibiotic course either completed during admission or prescribed at the time of discharge. MRSA risk factors included prior positive culture with MRSA within the last year, hospitalization with IV antibiotics within 90 days, intravenous drug use, or hemodialysis. Pseudomonal risk factors included prior positive culture with P. aeruginosa within the last year or hospitalization with IV antibiotics within 90 days. Results: In 2021, 260 unique patients were admitted with suspected diabetic foot infections or lower-extremity osteomyelitis. 68 patients had >1 admission. Empiric anti-MRSA and antipseudomonal therapy was administered to 224 (86%) and 214 (82%) patients, respectively. Definitive anti-MRSA and antipseudomonal therapy was administered to 76 (30%) and 51 (20%) patients, respectively. Of the 195 patients who had wound cultures, 29 (15%) and 18 (9%) had positive cultures for MRSA and P. aeruginosa respectively (Fig.). The negative predictive value of MRSA risk factors for predicting a negative culture with MRSA was 91%. The negative predictive value of pseudomonal risk factors for predicting a negative culture with P. aeruginosa was 95%. Conclusions: Our data suggest an opportunity for substantial reductions in empiric anti-MRSA and antipseudomonal therapy for diabetic foot infection and lower-extremity osteomyelitis. The absence of MRSA and pseudomonal risk factors was reasonably good at predicting the absence of a positive culture with these organisms.
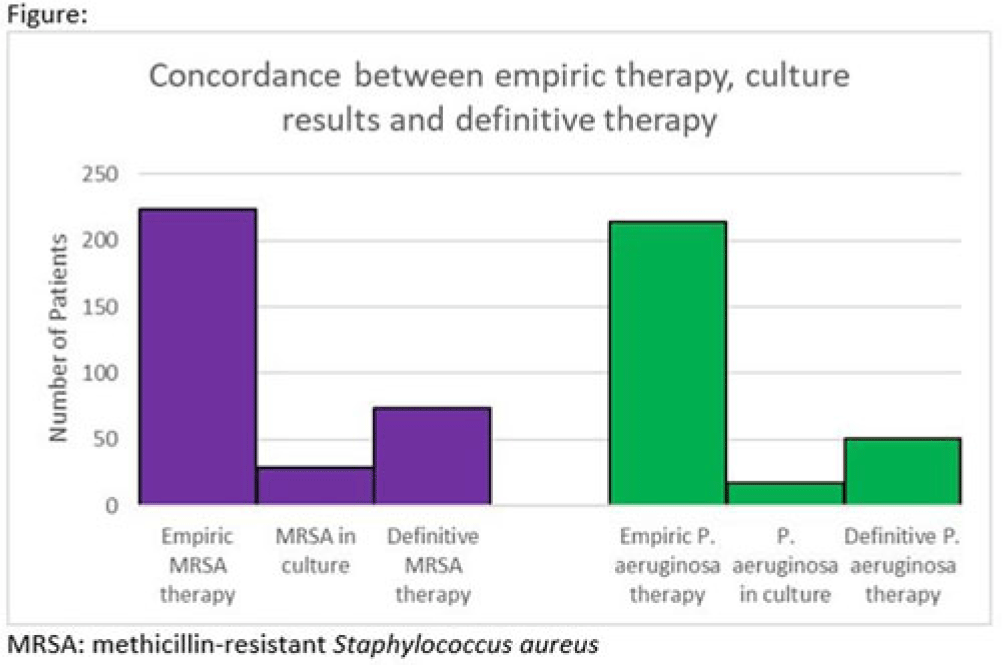
Disclosure: None
Original Article
Clinical impact of a multiplex rapid diagnostic pneumonia panel in critically ill patients
- Jayda N. Esplund, Alex D. Taylor, Tyler J. Stone, Elizabeth L. Palavecino, Abdullah Kilic, Vera P. Luther, Christopher A. Ohl, James R. Beardsley
-
- Published online by Cambridge University Press:
- 09 January 2023, e5
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To evaluate the clinical impact of the BioFire FilmArray Pneumonia Panel (PNA panel) in critically ill patients.
Design:Single-center, preintervention and postintervention retrospective cohort study.
Setting:Tertiary-care academic medical center.
Patients:Adult ICU patients.
Methods:Patients with quantitative bacterial cultures obtained by bronchoalveolar lavage or tracheal aspirate either before (January–March 2021, preintervention period) or after (January–March 2022, postintervention period) implementation of the PNA panel were randomly screened until 25 patients per study month (75 in each cohort) who met the study criteria were included. Antibiotic use from the day of culture collection through day 5 was compared.
Results:The primary outcome of median time to first antibiotic change based on microbiologic data was 50 hours before the intervention versus 21 hours after the intervention (P = .0006). Also, 56 postintervention regimens (75%) were eligible for change based on PNA panel results; actual change occurred in 30 regimens (54%). Median antibiotic days of therapy (DOTs) were 8 before the intervention versus 6 after the intervention (P = .07). For the patients with antibiotic changes made based on PNA panel results, the median time to first antibiotic change was 10 hours. For patients who were initially on inadequate therapy, time to adequate therapy was 67 hours before the intervention versus 37 hours after the intervention (P = .27).
Conclusions:The PNA panel was associated with decreased time to first antibiotic change and fewer antibiotic DOTs. Its impact may have been larger if a higher percentage of potential antibiotic changes had been implemented. The PNA panel is a promising tool to enhance antibiotic stewardship.
COVID-19
SG-APSIC1208: Association between severity of COVID-19 pneumonia and vaccination status in a tertiary-care teaching hospital in Malaysia
- Sasheela Sri La Sri Ponnampalavanar, Anjanna Kukreja, Sazali Basri, Sheron Sir Loon Goh, Syifa’ Ahmad Faisol, Reggina Chong Syin Tze, YiShi Ong, Anisa Salleh, SharifahFaridah Syed Omar, Zuhairah Mohd Razali, Adeeba Kamarulzaman
-
- Published online by Cambridge University Press:
- 16 March 2023, p. s2
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background and objectives: Since the introduction of the COVID-19 vaccine through the National COVID-19 Immunization Program in Malaysia in February 2021, the number of cases of severe COVID-19 and mortality have progressively decreased. We explored the association between vaccination status, type of vaccine, and the highest COVID-19 clinical category. Methods: Patients were recruited via the electronic medical record (EMR) at University Malaya Medical Centre (UMMC) from July 2021 onward. Included patients were aged ≥18 years old with positive SARS-CoV-2 RT-PCR results from respiratory samples (naso-oropharyngeal swab, saliva, or sputum). Patient demographic data, COVID-19 clinical category, vaccination status, and type of vaccine received were recorded. Results: In total, 1,391 positive SARS-CoV-2 PCR results were reviewed; 1,188 patients (85%) with complete data were analyzed. These patients’ median age was 50 years. The proportions of patients COVID-19 clinical categories were as follows: category 1 (4.04%), category 2 (28.37%), category 3 (10.7%), category 4 (30.6%), and category 5 (2.6%). The mortality rate was 21.5%. As of July 2021, only 16.8% of patients were fully vaccinated, 30.3% were vaccinated, 31.5% unvaccinated, and 21.5% had unknown vaccination status. In total 364 patients with category 4 COVID-19 (4.4%; P < .001) were fully vaccinated and no patients who were fully vaccinated had category 5 COVID-19 (P = .011). Furthermore, 40.8% of patients who died had unknown vaccination status (P < .01); 28.1% of patients who died were unvaccinated (P = .015); 25.3% of patients who died were partially vaccinated (P = .036); and 0.4% of patients who died were fully vaccinated (P < .001). For category 4 and 5 illness and death, there were no significant differences between the type of vaccine received (Pfizer-BioNTechR, Astra ZenecaR and Coronavac/SinovacR) and severe COVID-19. Conclusions: The completion of 2 doses of government-approved COVID-19 vaccination is paramount in preventing severe COVID-19 disease and death. Rapid rollout and equitable distribution of vaccination should be initiated. Vaccine hesitancy should be promptly addressed to ensure vaccination uptake.
Original Article
Multinational prospective cohort study of rates and risk factors for ventilator-associated pneumonia over 24 years in 42 countries of Asia, Africa, Eastern Europe, Latin America, and the Middle East: Findings of the International Nosocomial Infection Control Consortium (INICC)
- Victor Daniel Rosenthal, Zhilin Jin, Ziad A. Memish, Camilla Rodrigues, Sheila Nainan Myatra, Mohit Kharbanda, Sandra Liliana Valderrama-Beltran, Yatin Mehta, Mohammad Abdellatif Daboor, Subhash Kumar Todi, Guadalupe Aguirre-Avalos, Ertugrul Guclu, Chin Seng Gan, Luisa Fernanda Jiménez Alvarez, Rajesh Chawla, Sona Hlinkova, Rajalakshmi Arjun, Hala Mounir Agha, Maria Adelia Zuniga Chavarria, Narangarav Davaadagva, Mat Nor Mohd Basri, Katherine Gomez, Daisy Aguilar De Moros, Chian-Wern Tai, Alejandro Sassoe Gonzalez, Lina Alejandra Aguilar Moreno, Kavita Sandhu, Jarosław Janc, Mary Cruz Aleman Bocanegra, Dincer Yildizdas, Yuliana Andrea Cano Medina, Maria Isabel Villegas Mota, Abeer Aly Omar, Wieslawa Duszynska, Souad BelKebir, Amani Ali El-Kholy, Safaa Abdulaziz Alkhawaja, George Horhat Florin, Eduardo Alexandrino Medeiros, Lili Tao, Nellie Tumu, May Gamar Elanbya, Reshma Dongol, Vesna Mioljević, Lul Raka, Lourdes Dueñas, Nilton Yhuri Carreazo, Tarek Dendane, Aamer Ikram, Souha S. Kanj, Michael M. Petrov, Asma Bouziri, Nguyen Viet Hung, Vladislav Belskiy, Naheed Elahi, María Marcela Bovera, Ruijie Yin
-
- Published online by Cambridge University Press:
- 09 January 2023, e6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Rates of ventilator-associated pneumonia (VAP) in low- and middle-income countries (LMIC) are several times above those of high-income countries. The objective of this study was to identify risk factors (RFs) for VAP cases in ICUs of LMICs.
Design:Prospective cohort study.
Setting:This study was conducted across 743 ICUs of 282 hospitals in 144 cities in 42 Asian, African, European, Latin American, and Middle Eastern countries.
Participants:The study included patients admitted to ICUs across 24 years.
Results:In total, 289,643 patients were followed during 1,951,405 patient days and acquired 8,236 VAPs. We analyzed 10 independent variables. Multiple logistic regression identified the following independent VAP RFs: male sex (adjusted odds ratio [aOR], 1.22; 95% confidence interval [CI], 1.16–1.28; P < .0001); longer length of stay (LOS), which increased the risk 7% per day (aOR, 1.07; 95% CI, 1.07–1.08; P < .0001); mechanical ventilation (MV) utilization ratio (aOR, 1.27; 95% CI, 1.23–1.31; P < .0001); continuous positive airway pressure (CPAP), which was associated with the highest risk (aOR, 13.38; 95% CI, 11.57–15.48; P < .0001); tracheostomy connected to a MV, which was associated with the next-highest risk (aOR, 8.31; 95% CI, 7.21–9.58; P < .0001); endotracheal tube connected to a MV (aOR, 6.76; 95% CI, 6.34–7.21; P < .0001); surgical hospitalization (aOR, 1.23; 95% CI, 1.17–1.29; P < .0001); admission to a public hospital (aOR, 1.59; 95% CI, 1.35-1.86; P < .0001); middle-income country (aOR, 1.22; 95% CI, 15–1.29; P < .0001); admission to an adult-oncology ICU, which was associated with the highest risk (aOR, 4.05; 95% CI, 3.22–5.09; P < .0001), admission to a neurologic ICU, which was associated with the next-highest risk (aOR, 2.48; 95% CI, 1.78–3.45; P < .0001); and admission to a respiratory ICU (aOR, 2.35; 95% CI, 1.79–3.07; P < .0001). Admission to a coronary ICU showed the lowest risk (aOR, 0.63; 95% CI, 0.51–0.77; P < .0001).
Conclusions:Some identified VAP RFs are unlikely to change: sex, hospitalization type, ICU type, facility ownership, and country income level. Based on our results, we recommend focusing on strategies to reduce LOS, to reduce the MV utilization ratio, to limit CPAP use and implementing a set of evidence-based VAP prevention recommendations.
COVID-19
SG-APSIC1053: Detection of SARS-COV-2 in nasopharyngeal swags with MALDI-TOF MS and machine learning
- Irina Kadyrova, Svetlana Kolesnichenko, Ilya Korshukov, Yevgeniya Kolesnikova, Valentina Barkhanskaya, Alyona Lavrinenko, Aidana Sultanbekova, Sergey Yegorov, Dmitriy Babenko
-
- Published online by Cambridge University Press:
- 16 March 2023, pp. s2-s3
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objectives: The widespread distribution of SARS-CoV-2 and its high contagiousness pose a challenge for researchers seeking to develop a rapid and cost-effective screening method to identify carriers of this virus. RT-PCR is considered the gold standard for detecting viral RNA in nasopharyngeal swabs, but it is time-consuming and requires constant changes in the primer composition due to the mutation of SARS-CoV-2 strains. We propose a method for the detection of SARS-CoV-2 in nasopharyngeal swabs using MALDI-TOF MS and machine learning. Methods: Nasopharyngeal swabs from patients with PCR-confirmed COVID-19 and control participants were tested (130 and 80 swabs, respectively) with MALDI-TOF MS MicroFlex LT using the HCCA matrix. MALDI spectra were preprocessed in R version 4.1.2 software with the MALDIquant R package using the workflow: sqrt transformation, wavelet smoothing, SNIP-based base removal, and PQN intensity calibration. Peaks were detected with MAD algorithms with following Peak alignment on the following parameters: minFreq 70% and tolerance 0.005. Machine learning was performed with the rtemis r package on GLM, random forest, and XGBoost models. Results: These models were characterized by specificity, sensitivity, and F1 score. GLM models (specificity 1 and sensitivity 0.5) showed a low F1 score of 0.71. However, the random forest and XGBoost models demonstrated sensitivity, specificity, and F1 score equaling 1. Conclusions: We propose a screening method for SARS-CoV-2 detection (sensitivity 1 and specificity 1). This methodology combines the analysis of nasopharyngeal swab samples using MALDI-TOF-MS with machine learning. It is suitable for screening patients with COVID-19 at the first stages of diagnosis. Random forest and XGBoost models demonstrated sensitivity, specificity, and F1 scores equaling 1.
Poster Presentation - Top Poster Award
Antibiotic Stewardship
Inpatient pediatric antimicrobial use for respiratory infections during the RSV surge
- Aaron Hunt, Rodrigo Burgos, Alfredo Mena Lora
-
- Published online by Cambridge University Press:
- 29 September 2023, pp. s4-s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: In the United States, pneumonia causes >100,000 pediatric hospitalizations annually. On November 4, 2022, the CDC issued a Heath Advisory concerning an upcoming surge of respiratory illnesses including SARS-CoV-2, influenza, and respiratory syncytial virus (RSV). Differentiating between viral and bacterial causes is challenging and can lead to antimicrobial overuse. Currently, tools are being developed to distinguish between viral and bacterial pneumonia. The VALS-DANCE Pneumonia Etiology Predictor (PEP) provides clinical scoring criteria (Fig. 1) to determine probable cause of pneumonia with 93.1% sensitivity for bacterial pneumonia. Scores >11 have a >25% likelihood of having bacterial etiology. Given that antimicrobial exposure increases resistance rates, disrupts natural flora, and increases the risk of side effects, a core goal of researchers is to develop ways to promote stewardship and reduce inappropriate use. We assessed the patterns of use for antimicrobials in pediatric patients admitted with pneumonia at our institution. Methods: This retrospective review included pediatric cases admitted to an urban safety-net community hospital from July 22, 2022, to December 16, 2022. A daily list of all patients receiving antimicrobials was reviewed, and pediatric patients with diagnosis of a respiratory infection were included. Patients with additional indications for antimicrobial therapy, diagnosis of bronchitis, incomplete records, or without complete information were excluded from the scoring criteria. The primary objective was to assess the appropriateness of antimicrobial use for pneumonia, defined as use consistent with PEP scoring recommendations. Results: Of 53 patients reviewed, 37 met inclusion criteria. Of 37 patients, 22 (59.5%) met study criteria for appropriate therapy. The 15 patients (40.5%) who were inappropriate for treatment received an average of 4.67 ± 1.91 days of antibiotics. Of these 15 patients, 11 (73.3%) also had a positive viral test, further increasing the likelihood of a viral etiology. This subgroup had an average antibiotic exposure of 4.27 ± 1.79 days. Documented rationale for therapy included severity of illness (4 of 11), radiograph consolidation (4 of 11), and provider disagreement with radiograph interpretation (3 of 11). Conclusions: Pediatric respiratory infections represent a significant opportunity for antimicrobial stewardship. In this study, as many as 40% of pediatric patients may have received unnecessary antibiotic exposure. Use of the VALS-DANCE criteria may help clinicians identify patients with low likelihood of bacterial infection and reduce antimicrobial use. The national surge of viral infections serves to highlight the vital importance of appropriate diagnostic stewardship.
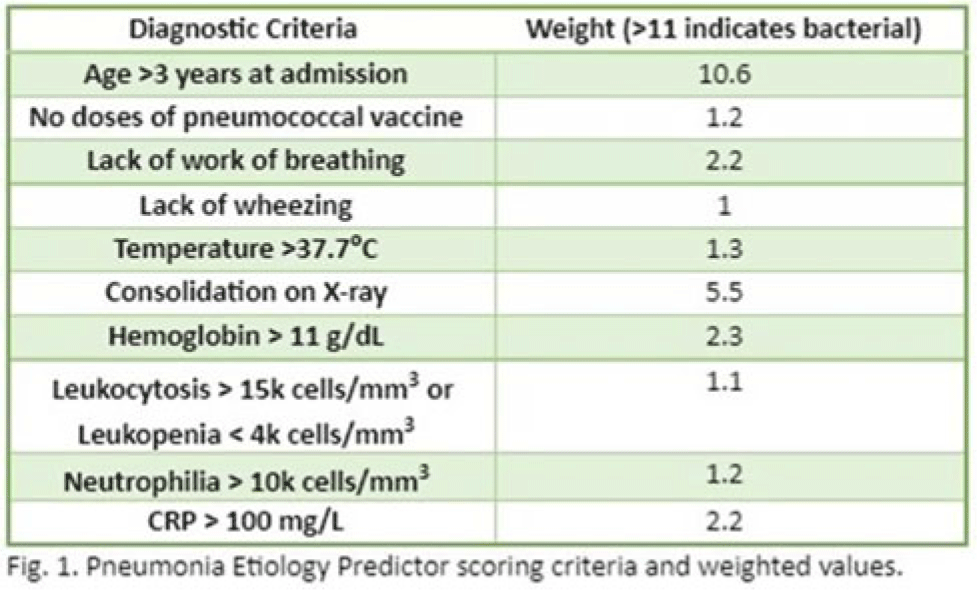
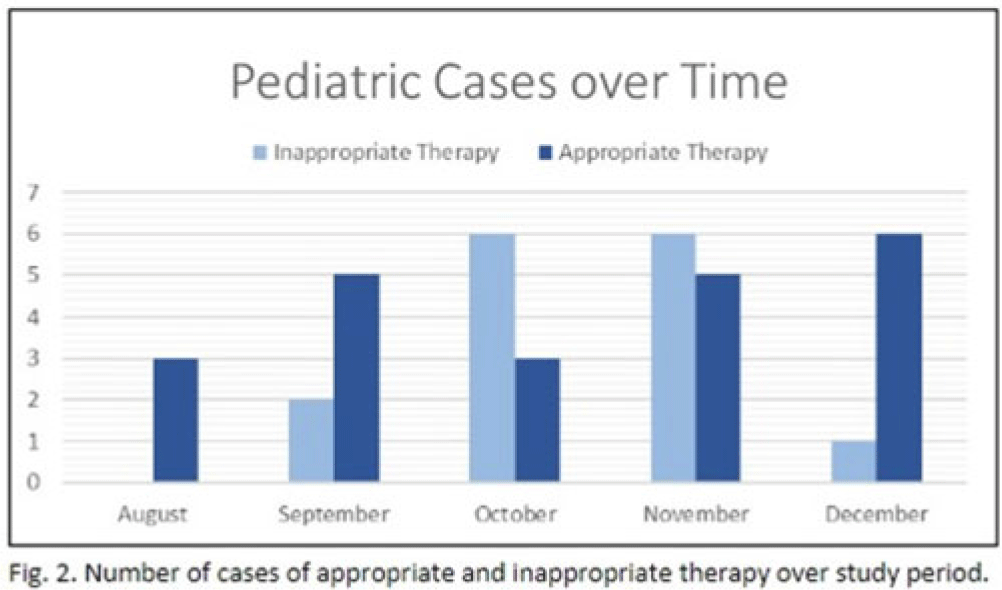
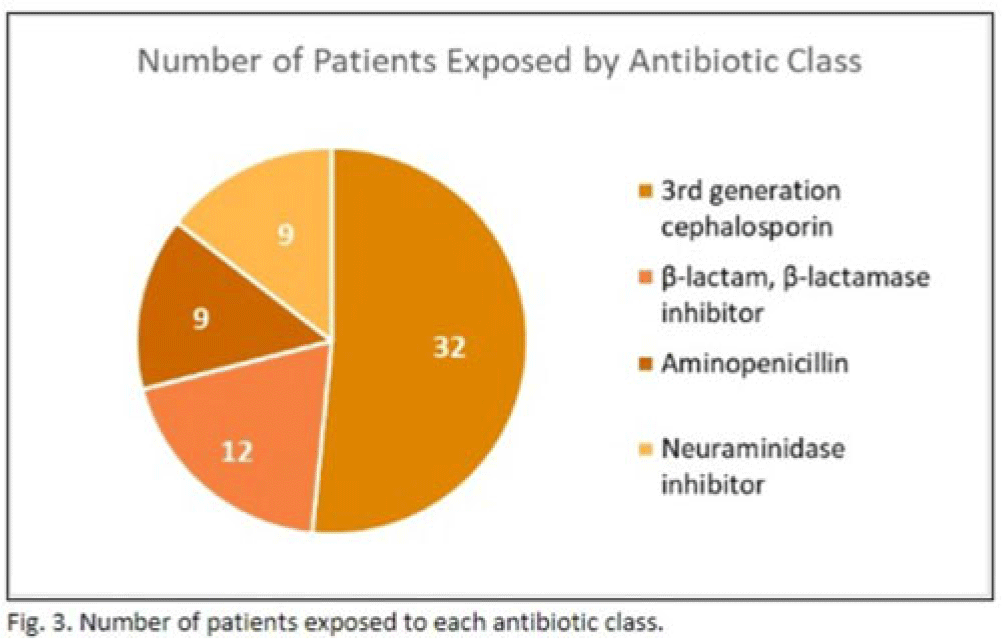
Disclosure: None
Research Brief
Detection of SARS-CoV-2 from combined nasal/rectal swabs
- Adriana M. Airo, Kevin R. Barker, Matthew P. Muller, Linda R. Taggart, Karel Boissinot, Ramzi Fattouh, Bridget Tam, Larissa M. Matukas
-
- Published online by Cambridge University Press:
- 09 January 2023, e7
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Poster Presentation - Top Poster Award
C. difficile
Integrated efficacy analysis from phase 3 studies of investigational microbiome therapeutic, SER-109, in recurrent Clostridioides difficile infection
- Matthew Sims, Michael Silverman, Thomas Louie, Elaine Wang, Colleen Kraft, Mayur Ramesh, Tatiana Bogdanovich, Kelly Brady, David Lombardi, Asli Memisoglu, Ananya De, Brooke Hasson, Christine Lee, Paul Feuerstadt, Darrell Pardi, Colleen Kelly, Peter Daley, Godson Oguchi, Barbara McGovern, Lisa Von Moltke
-
- Published online by Cambridge University Press:
- 29 September 2023, p. s5
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antibiotics alone are often insufficient to treat recurrent C. difficile infection (rCDI) because they have no activity against C. difficile spores that germinate within a disrupted microbiome. SER-109, an investigational, oral, microbiome therapeutic comprised of purified Firmicutes spores, was designed to reduce rCDI through microbiome repair. We report an integrated efficacy analysis through week 24 for SER-109 from phase 3 studies, ECOSPOR III and ECOSPOR IV. Methods: ECOSPOR III was a randomized, placebo-controlled phase 3 trial conducted at 56 US or Canadian sites that included 182 participants with ≥2 CDI recurrences, confirmed via toxin EIA testing. Participants were stratified by age (<65 years or ≥65 years) and antibiotic regimen (vancomycin, fidaxomicin) and were randomized 1:1 to placebo or SER-109 groups. ECOSPOR IV was an open-label, single-arm study conducted at 72 US or Canadian sites including 263 participants with rCDI enrolled in 2 cohorts: (1) rollover participants from ECOSPOR III who experienced on-study recurrence diagnosed by toxin EIA (n = 29) and (2) participants with ≥1 CDI recurrence (diagnosed by PCR or toxin EIA), inclusive of the current episode (n = 234). In both studies, the investigational product was administered orally as 4 capsules over 3 consecutive days following symptom resolution after standard-of-care antibiotics. The primary efficacy end point was rCDI (recurrent toxin-positive diarrhea requiring treatment) through week 8. Other end points included CDI recurrence rates and safety through 24 weeks. Results: These 349 participants received at least 1 dose of SER-109 in ECOSPOR III or ECOSPOR IV (mean age 64.2; 68.8% female). Overall, 77 participants (22.1%) enrolled with their first CDI recurrence. Four participants received blinded SER-109 in ECOSPOR III followed by a second dose of open-label SER-109 in ECOSPOR IV. Overall, the proportion of participants who received any dose of SER-109 with rCDI at week 8 was 9.5% (33 of 349; 95% CI, 6.6 %–13.0%), and the CDI recurrence rate remained low through 24 weeks (15.2%, 53 of 349; 95% CI, 11.6%–19.4%), corresponding to sustained clinical response rates of 90.5% (95% CI, 87.0%–93.4%) and 84.8% (95% CI, 80.6%–88.4%), respectively (Fig. 1). Most rollover participants (25 of 29, 86.2%) were from the placebo arm; 13.8% had rCDI by week 8. Conclusions: In this integrated analysis, the rates of rCDI were low and durable in participants who received the investigational microbiome therapeutic SER-109, with sustained clinical response rates of 90.5% and 84.8% at weeks 8 and 24, respectively. These data further support the potential benefit of microbiome repair with SER-109 following antibiotics for rCDI to prevent recurrence in high-risk patients.
Financial support: This study was funded by Seres Therapeutics.
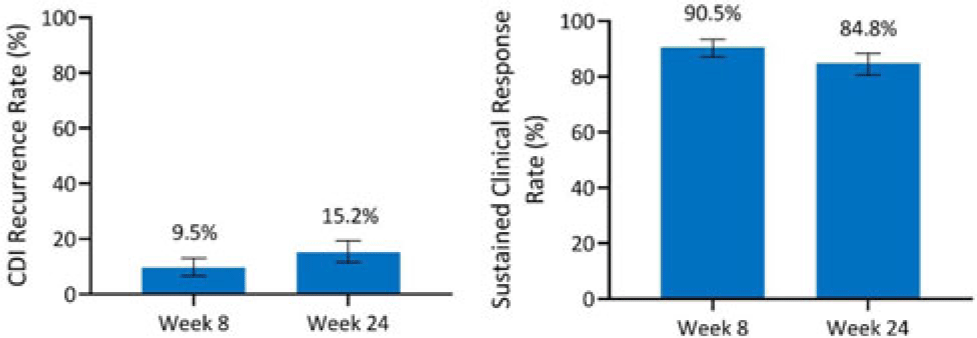
Disclosure: None














